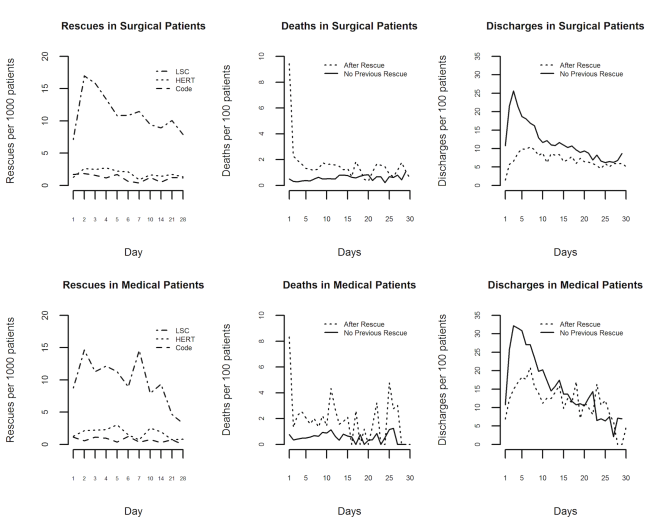
A comprehensive system-level performance analysis of an existing rescue system was conducted using a systems analysis approach to characterize:
- Patient demographics.
- Rescue activation types and locations.
- Temporal patterns of activation.
- Associations of patient factors, including complications, with post-rescue care disposition and outcomes.
The study builds upon previous work highlighting that early recognition of changes in the patient state is a key factor in preventing FTR events and underscores the importance of bringing resources and tools (for example, continuous monitoring and LSCs) to the bedside to enhance early recognition.
Results showed that increases in bedside consultations (20% per year) were found with increased rescue activations during periods of resource limitations and changes (for example, shift changes and weekends).
- Cardiac arrest, respiratory failure, and sepsis complications present the highest risk for rescue and death.
- Distributions of rescue and death incidence by day of patient stay may suggest opportunities for earlier recognition.
While results may not be generalizable to other hospitals with different rescue systems, the approach and methods applied can be used by other institutions to understand performance and allow rational incremental improvements to this complex care delivery system.
McGrath S, MacKenzie T, Perreard I, Blike G. Characterizing rescue performance in a tertiary care medical center: a systems approach to provide management decision support. BMC Health Serv Res. 2021 Aug 20;21(1):843. Doi: 10.1186/s12913-021-06855-w. PMID: 34416882; PMCID: PMC8379722